Oxford University researchers across the globe are working to beat Malaria. Now, a team of Oxford scientists in the UK and Kenya, working with colleagues in three Swiss institutes, have found two people who could reveal a new approach to targeting the malaria parasite.
Malaria still claims over 400,000 lives every year, mostly due to infection by a single species of malaria parasite called Plasmodium falciparum. However, people living in areas where malaria is common naturally acquire immunity that protects them during their adult lives. So one route to finding new vaccines against malaria is by getting down to the molecular level to identify the processes behind this natural immune response.
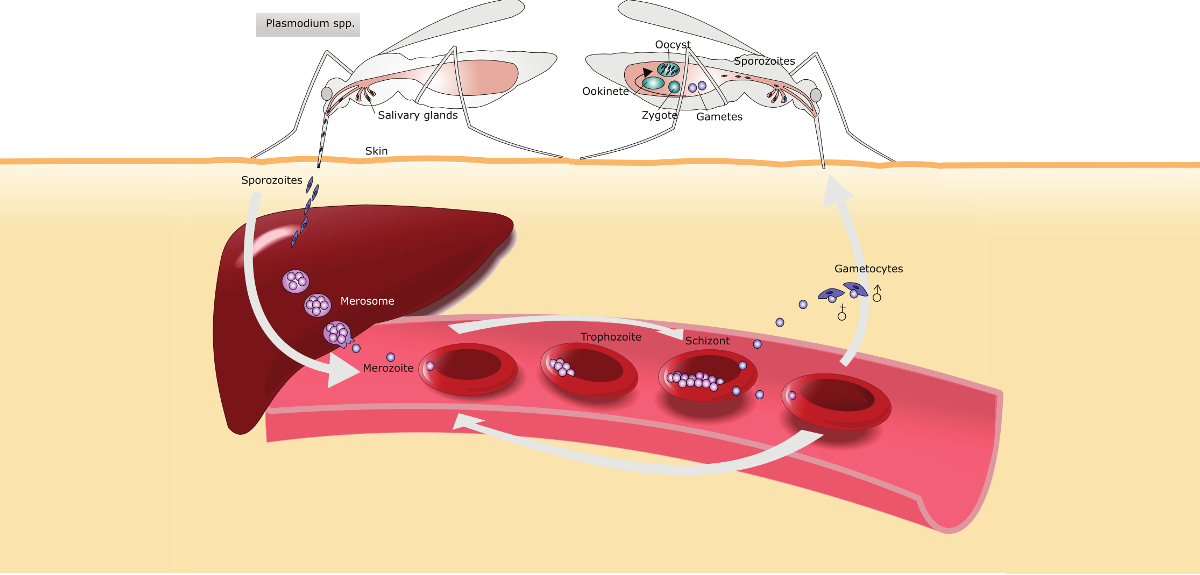
Severe, life-threatening malaria occurs during a stage in the Plasmodium falciparum parasite life-cycle when these parasites infect and hide within red blood cells. Several previous studies suggested that a major component of the protective immune response is directed against molecules called 'variant surface antigens' that parasites insert into the surface of infected red blood cells. These molecules are used by parasites to manipulate the infected cells so that they stick to the linings of blood vessels that supply organs in the body including the brain. If large numbers of parasite-infected red blood cells accumulate in the brain, it causes 'cerebral malaria' – a life-threatening coma.
Several molecular 'families' of variant surface antigens are manufactured by Plasmodium falciparum. Despite the key role that they play both as targets of naturally acquired immunity and in the development of severe malaria they are often regarded as unsuitable vaccine candidates because of their diversity. However, finding antibodies that cross react with a broad range of Plasmodium falciparum variant surface antigens from different individuals would potentially lead to the development of new interventions against malaria.
Variant surface antigens include PfEMP1, the most prominent, as well as RIFINs and STEVOR. While previous research emphasis has been placed on PfEMP1, the team found two rare individuals who carried antibodies that recognize not PfEMP1, but RIFINs. The reports online this week in the journal Nature.
The team found that at the molecular level, this reactivity in the antibodies was brought about through independent and novel events that occurred during their natural generation in the body, in which migration and insertion of DNA occurred from a non-antibody gene called LAIR1.
The researchers suggest that finding the molecular shape that these antibodies recognize on RIFINs may lead to a potential vaccine. However, they caution that there is still a need for more research before we know if such a vaccine would be effective.