If you ever wonder where the NHS' drugs budget is going, a new website could help answer your questions. Prescribing data from NHS GP practices across England can now be scrutinised online to see how responsive they are to cost-efficiency and patient safety recommendations.
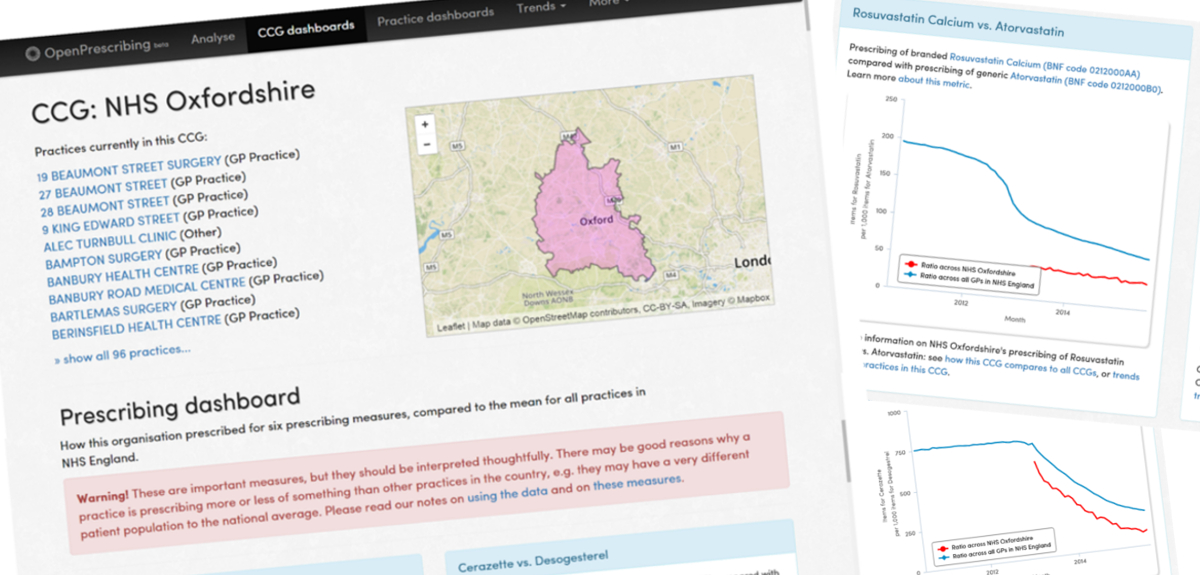
Openprescribing.net is the first website of its kind to enable health professionals, patients and the public to easily explore patterns of prescribing nationally, in Clinical Commissioning Groups (CCG) and by individual GP practices.
The project has been developed by researchers at the University of Oxford’s Nuffield Department of Primary Care Health Sciences in collaboration with epidemiologists, doctors and coders and turns raw data from the NHS into a fully functioning live service. It provides feedback on every prescribed drug through easy-to-read graphs and dashboards and aims to make NHS prescribing data clear, open and accessible to everyone. The project has received funding and additional collaborative support from the West of England Academic Health Science Network.
Dr Ben Goldacre, a Senior Research Fellow at the University of Oxford, who leads the project, said: 'If we want to improve standards in healthcare we need good data that can be accessed and interpreted quickly. With a very small amount of funding we’ve taken prescribing data from the NHS and made it open to everyone and free to access. Doctors and others in the NHS can get useful simple feedback on prescribing behaviours that are potentially wasteful, or even harmful. Crucially this service is fully open: that means everyone can see the data and use it, whether they are a practice manager, a patient, a journalist, a member of the public, a doctor, or a researcher.
'Presenting this data in a user-friendly format has the potential to save the NHS phenomenal amounts of money. By giving individual GPs, practice managers and clinical commissioning groups the power to scrutinise their efficiency, they can start to routinely monitor their performance against national or regional trends. OpenPrescribing.net lets anyone spot outliers, so we can see who is prescribing an unusually high quantity of antibiotics, or whether a practice or CCG is responding to recommendations to prescribe generic drugs over their branded equivalents, which is a top cost-saving tactic in the NHS.'
Currently in early 'beta' phase, the site can produce dashboards, maps and graphs on any drug the user selects. There also six standard measures that can be rapidly visualised for any CCG or practice, to illustrate the best ways the service can be used, each with an explanation of what they mean. Future development work seeks to add around 100 such standard measures, chosen in consultation with healthcare professionals and patients, and many more innovative new features, though additional funding is needed to make this possible.
Using the website comes with a caveat, however. 'It's important to be thoughtful about how you interpret this data,' warns Ben Goldacre. 'If any one practice is using a high or low quantity of a particular drug, that could mean that the doctors' decision making processes are different, or it could mean that their patients are different. For example, if a practice is prescribing a lot of valium, that may mean the doctors there have a lower threshold for giving out such drugs; or it could mean that the practice specialises in providing services for patients with substance misuse problems.'
The site contains advice on interpreting the data, and the researchers have developed new statistical methods for identifying outliers more accurately which will be implemented on the site and published shortly.
Openprescribing.net utilises raw data on GP practice prescribing from the Health and Social Care Information Centre. This is updated monthly and has been in the public domain under an Open Government License since 2012, but until now has yet to be offered in a format that allows for quick and easy reporting at the practice, CCG or national level.
The site has been supported by the West of England AHSN. Peter Brindle, Commissioning Evidence-Informed Care Lead at the AHSN: said: 'Ever increasing pressures on our healthcare system has led to a major drive for innovation in how the health services go about their daily business and to underpin new models of healthcare delivery with evidence.
'This is exactly what we have set out to do with OpenPrescribing and the potential of this approach is vast. CCGs and practices can now easily compare themselves with others, and this can trigger ideas for projects to improve patient care and reduce waste. They can also ensure that medications, which should be used for certain conditions as stipulated by NICE guidelines, are being prescribed and less effective medicines are not.
'Furthermore patients can use the platform to see how widely the medications they are taking are being prescribed by their practice and how that compares with other practices.'